Prostate Cancer
Prostate cancer is a malignant tumour that grows in the prostate, a walnut-sized gland below the bladder in men that produces semen. Most prostate cancers are slow-growing but there are aggressive cases, and the cancer can spread to other parts of the body, especially the bones and lymph nodes.
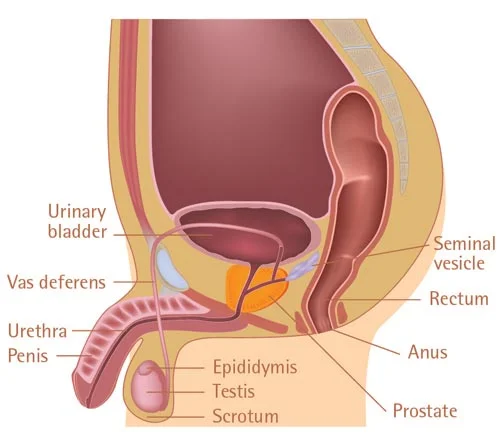
In many cases, there are no symptoms, and it is believed that as many as 80 per cent of men who reach the age of 80 will have prostate cancer. As most cases are slow-growing, many will, in fact, die of other ailments of old age without ever realising that they have the cancer.
When symptoms do emerge in more advanced stages, they include weight loss, pelvic pain, back or hip pain and urinary difficulties, such as burning or pain during urination, the inability to urinate or blood in the urine.
Screening Tests for Early Detection
- Digital Rectal Examination (DRE) - This may be carried out by a doctor. Using a gloved finger to examine the rectum, he may be able to feel a lump or growth in the prostate.
- Prostate-Specific Antigen (PSA) Test – This is the most common initial test for prostate cancer. It tests the level of PSA – a protein produced by the cells in the prostate gland – in the blood. The higher the level, the more likely cancer is present, although other factors may cause an elevated PSA reading as well.
Test to Diagnose Prostate Cancer
- Prostate Biopsy - If prostate cancer is suspected, a biopsy – removal of sample tissue – is carried out, after which, if the result is positive, a bone scan, CT or MRI scan of the pelvis may be needed to determine the extent of the tumour.
- Transrectal Ultrasound – This uses sound waves to visualise the prostate gland. This is most often used during a biopsy to guide the needles into the part of the prostate gland where tumour is suspected.
Tests After Cancer Is Diagnosed
- PSA Levels – Once cancer is diagnosed, PSA levels may help determine its extent. If PSA levels are lower than 20ng/mL, it is likely that the cancer has not spread to distant sites. PSA levels over 40ng/mL are strong indicators that cancer has spread to other parts of the body.
- Tests for Metastasis – If the biopsy indicates cancer, other tests will be done to determine how far the cancer has spread. Bone scans and x-rays may reveal whether the cancer has invaded the bones. Computed tomography (CT) or magnetic resonance imaging (MRI) scans can further pinpoint the location of the cancer.
Grading
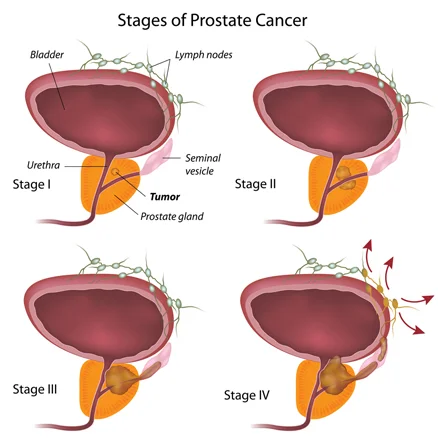
Prostate cancer is graded according to the Gleason system, which measure how well or how poorly organised the cancer cells are, under the microscope.
Grade 1: Cancerous tissue looks much like normalprostate tissue.
Grade 2 to 4: Some cells look like normal cells, some do not.With features that vary in between the two extremes.
Grade 5: Cancer cells and growth patterns look very abnormal.
Since prostate cancers often have areas with different grades, a grade is assigned to the 2 areas that make up most of the cancer. These 2 grades are added together to yield the Gleason score between 6 and 10.
A Gleason score of 6 or less indicates a less aggressive cancer. A score of 7 and above is considered aggressive and more likely that the cancer will grow and spread quickly.
In some cases, because prostate cancer may take many years to progress, and treatment does have its risks, doctors may choose to simply monitor the tumour rather than treat it immediately. The indication for treatment therefore depends on many factors such as the extent of cancer, symptoms, age, and general health of the patient.
Localised Prostate Cancer
In patients with localised disease and who needs treatment, surgery and/or radiation, with or without hormonal treatment may be considered.
- Surgery – When treatment is decided on, it could include surgical removal of the prostate gland if the cancer is localised. Chances of a full recovery are high in such cases but possible side effects include urinary incontinence and impotence.
- Radiation Therapy – By using high-energy rays to target and kill cancer cells. This may also be used when the cancer is localised.
- Hormonal Therapy – Counters the effects of testosterone and may be used as an adjunct to surgery or radiation in patients with high risk features.
Advanced Prostate Cancer
In patients with advanced prostate cancer, many treatment options are now available.
- Hormonal Therapy – Counterstheeffectsoftestosteroneandmay be used to treat prostate cancers that have spread beyond the prostate gland. The range of approved hormonal treatment options is broad and many agents have been shown to be effective in controlling prostate cancer.
- Chemotherapy – Chemotherapy is used to alleviate symptoms of prostate cancer if other treatments ineffective, and can be given together with hormonal therapy.
- Radioactive Bone Isotope - This treatment is used to treat prostate cancers that have spread to the bones. These radioactive isotopes are similar to calcium and are taken up by bones. Once in the bones, it releases radiation to kill the cancer cells. And since cancer cells are more active than normal bones, they are more likely to take up the isotopes and thus more likely to be killed by the radiation released.
- Immunotherapy - Immunotherapy such as Sipuleucel-T are effective in prostate cancer. A patient’s own immune cells are collected and exposed to proteins intended to stimulate and direct them against prostate cancer cells. These immune cells are then returned back to patient to treat his prostate cancer.
What Is The Best Approach To Care?
The development of a treatment plan by a multi-disciplinary team – surgeons, pathologists, radiologists, medical and radiation oncologists, radiologists, social workers and nurses to diagnose, treat and manage the condition has shown to improve the outcome for patients with cancer.
Who is at Risk of Prostate Cancer and How Can One Prevent It?
Age is one factor, with men in their 40s having a risk of just one in 200,000, in their early 50s, it jumps to 12 per 100,000, while men in their 60s have a 12 out of 10,000 chance of being diagnosed with prostate cancer.
People, who are obese, eat excessive amounts of meat or food high in animal fat also have an increased risk of prostate cancer. Also in the higher-risk group are men with a family history of prostate cancer.
A healthy lifestyle, with lower meat consumption, therefore, goes a long way in helping to prevent prostate cancer as well as other cancers.

CanHOPE is a non-profit cancer counselling and support service provided by Parkway Cancer Centre, Singapore. CanHOPE consists of an experienced, knowledgeable and caring support team with access to comprehensive information on a wide range of topics in education and guidelines in cancer treatment.
CanHOPE provides:
- Up-to-date cancer information for patients including ways to prevent cancer, symptoms, risks, screening tests, diagnosis, current treatments and research available.
- Referrals to cancer-related services, such as screening and investigational facilities, treatment centres and appropriate specialist consultation.
- Cancer counselling and advice on strategies to manage side effects of treatments, coping with cancer, diet and nutrition.
- Emotional and psychosocial support to people with cancer and those who care for them.
- Support group activities, focusing on knowledge, skills and supportive activities to educate and create awareness for patients and caregivers.
- Resources for rehabilitative and supportive services.
- Palliative care services to improve quality of life of patients with advanced cancer.
The CanHOPE team will journey with patients to provide support and personalised care, as they strive to share a little hope with every person encountered.
