Colorectal (Colon) Cancer
Overview
What is Colorectal Cancer?
Colorectal cancer, commonly known as colon cancer or large intestine cancer, originates from the tissues of the colon (the longest part of the large intestine) or rectum (the last several inches of the large intestine before the anus).
How Common is Colorectal Cancer?
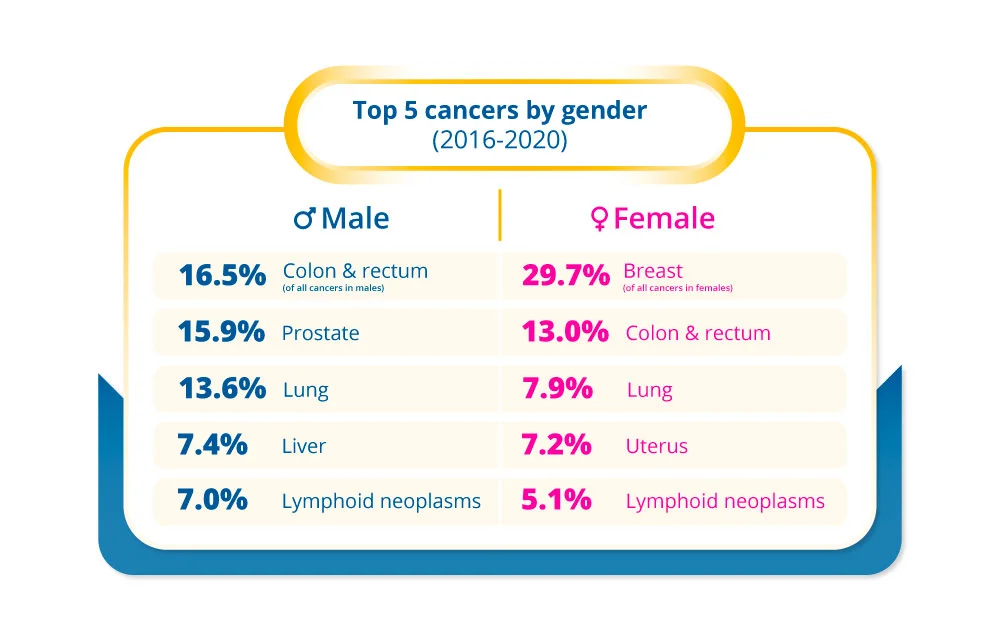
Colorectal cancer is one of the most common cancers. In Singapore, colorectal cancer is the most common cancer amongst males, accounting for almost 17% of all cancers in males, and second to breast cancer in females, making up 13% of all cancers in females1.
The good news is that the number of deaths from colorectal cancer has been decreasing over the last 15 years1. In part, this could be because more people are going for regular screening, which can detect colorectal cancers early2. Treatment for colorectal cancer has also improved. This means that patients can be treated more effectively2. Early detection of colorectal cancer can normally lead to a complete cure3.
Causes & Symptoms
What causes Colorectal Cancer?
There is no single cause of colorectal cancer, but it is likely a combination of genetic and environmental factors4. In most cases, colon cancers begin as a benign polyp that develops into a cancerous growth over a period of 5 to 10 years4.
Colorectal Cancer Risk Factors
While no one really knows the exact causes, we do know that people with certain risk factors are more likely than others to develop colorectal cancer. Studies have shown that people with the following risk factors are more likely to develop colorectal cancer5:
Colorectal polyps
Polyps are growths on the inner wall of the colon or rectum and is common in people over 50 years old. Most polyps are benign (not cancerous), but over time genetic changes can occur and some polyps (adenomas) can become cancerous.Inflammatory bowel disease
A person who has had a condition that causes inflammation of the colon (such as ulcerative colitis or Crohn’s disease) for many years is at an increased risk.Personal history of cancer
A person who has already had colorectal cancer before is more likely to develop colorectal cancer a second time. Also, women with a history of cancer of the ovary, uterus (endometrium), or breast are at a higher risk of developing colorectal cancer.Family history
Those who have one or more first-degree relative (parent, sibling or child) with colorectal cancer, are more likely than others to develop this disease, especially if your relative had the cancer at a young age.Lifestyle factors
Individuals who smoke, have a heavy alcohol intake, consume a diet that is high in fat and low in fibre (found in fruits and vegetables), are overweight or physically inactive are at an increased risk of colorectal cancer.Age
Colorectal cancer is more likely to occur as people get older. More than 90 percent of people with this disease are diagnosed after age 50 years and above6.
What are the Signs and Symptoms of Colorectal Cancer?
Colorectal cancer does not always cause symptoms, especially early in the disease.
Colorectal cancer symptoms may include7:
- Change in bowel habits (diarrhoea or constipation)
- Feeling that your bowel does not empty completely
- Finding blood (either bright red or very dark) in your stool
- Finding your stools are narrower than usual
- Frequently having gas pains or cramps, or feeling full or bloated
- Losing weight with no known reason
- Feeling very tired all the time
- Having nausea or vomiting
Other health problems can cause some of these symptoms. Additionally, it is important to note that early cancer does not usually cause pain.
If you have any of these symptoms, please consult your doctor. Remember that early diagnosis and treatment leads to better outcomes than those diagnosed at later stages of the cancer.
Diagnosis & Assessment
Diagnosis of Colorectal Cancer
If you have a symptom or screening results that suggest colorectal cancer, your doctor will investigate further to determine if you have cancer. Colorectal cancer can be detected through the following procedures and tests8:
Clinical history and examination
Your doctor will ask about your personal and family medical history and perform a physical examination for masses in your abdomen.Sigmoidoscopy
This test may be done if cancer of the rectum is suspected. Your doctor examines your rectum and lower part of the colon with a thin, rigid, lighted tube (sigmoidoscope) for any tumours.Colonoscopy
Your doctor examines your entire colon and rectum using a thin, flexible, lighted tube (colonoscope) with a video camera on the end. The tube is inserted through the anus and into the rectum and the colon.CT colonography
Also known as virtual colonoscopy, this procedure uses special X-ray equipment to obtain interior scans of the colon and rectum.
If abnormalities (such as polyps) are found, a biopsy may be required. Often, the abnormal tissue can be removed during colonoscopy or sigmoidoscopy. A pathologist then checks the tissue for cancer cells using a microscope.
How is Colorectal Cancer Assessed?
If the biopsy shows that cancer is present, your doctor needs to know the extent of the disease to plan the best treatment. The stage is based on whether the tumour has invaded nearby tissues, whether the cancer has spread and, if so, to what parts of the body.
Doctors describe colorectal cancer stages as9:
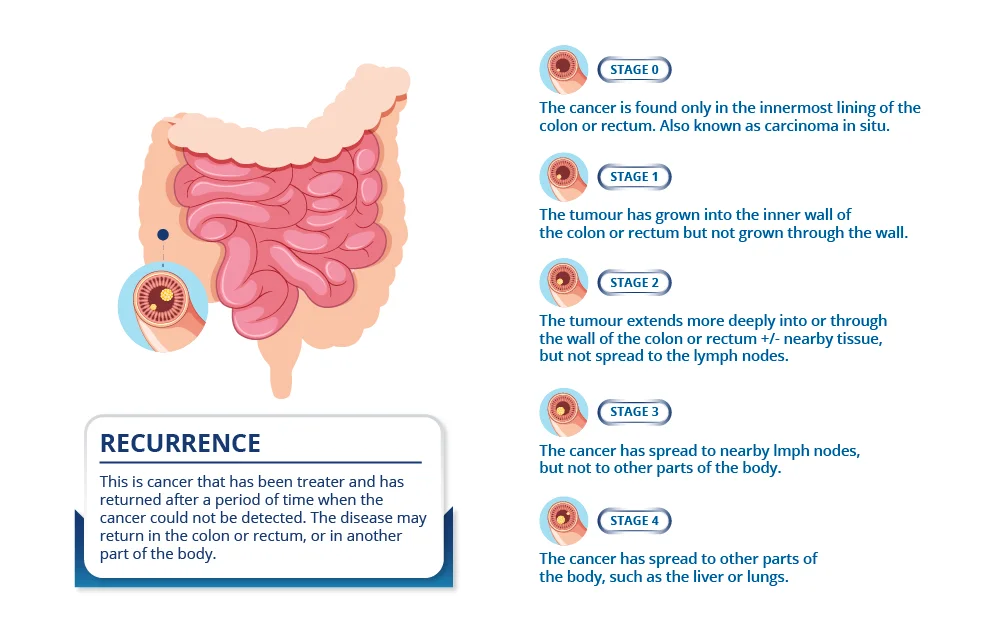
Treatment of Colorectal Cancer
Colorectal Cancer Treatment Options
In recent years, there has been great progress in treatments for colorectal cancer. In particular, there are now very good treatments for those with advanced disease.
What is most suitable depends on what kind of tumour, the location as well as patient characteristics2. Local treatments are typically suitable for early stage cancers, thus patients can be treated without affecting the rest of the body10. Systemic treatment typically involves the use of drugs, either delivered by mouth or directly into the bloodstream, to reach cancer cells around the body10.
Surgery
Colorectal cancer surgery involves the removal of tissues that contain the tumour and nearby tissues/lymph nodes. This may be done via laparoscopy (keyhole surgery) or laparotomy (open surgery).Chemotherapy
Chemotherapy involves the use of anticancer drugs to shrink/kill cancer cells. The drugs enter the bloodstream and therefore goes around the body. It is commonly prescribed for advanced (stage 3 or 4) cancers to control the cancer and occasionally stage 2 colon cancer after surgery to decrease the chance of recurrence.Targeted cancer therapy
Some people with colorectal cancer that has spread to other parts of the body may be given targeted therapy. Targeted therapies are drugs that block the growth and spread of cancer by interfering with specific molecules involved in tumour growth and spread.Radiation therapy
Radiation therapy (also called radiotherapy) uses high-energy rays to kill cancer cells. It affects cancer cells only in the treated area. It is used mainly in rectal cancer.
Colorectal Cancer Survival Rate
Early diagnosis of colorectal cancer saves lives. The earlier it is detected, the higher the likelihood for cure.3
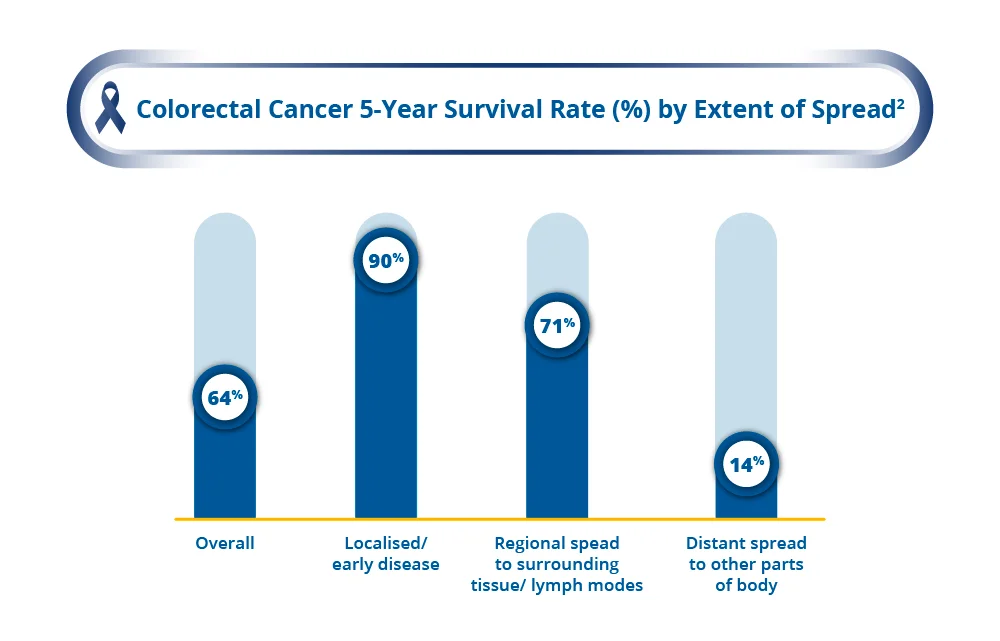
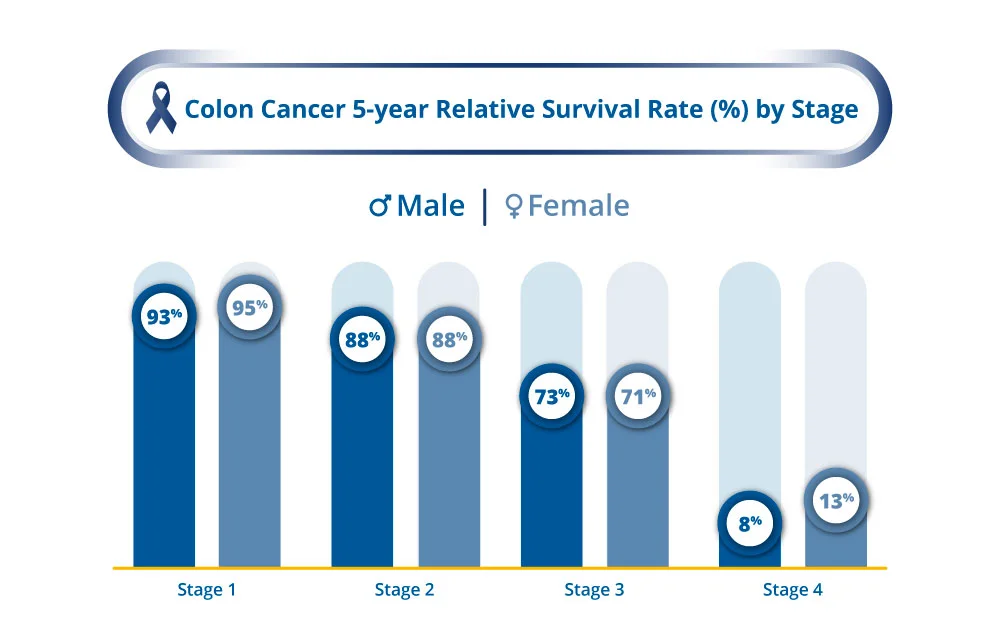
It is important to bear in mind that these rates are estimates and with continued advancements in treatment as well as screening methods, the survival rate for colorectal cancer is expected to continue to improve.
Prevention & Screening
Colorectal Cancer Screening
Screening tests are important! They help your doctor find polyps or cancer before you have symptoms. Early detection of colorectal cancer will also improve effectiveness of cancer treatment. The following screening tests can be used to detect polyps, cancer, or other abnormalities11:
Fecal Occult Blood Test (FOBT) or Fecal Immunochemical Tests (FIT)
Sometimes cancers or polyps bleed, and the FOBT or FIT can detect tiny amounts of blood in the stool. If this test detects blood, other tests are needed to find the source of the blood. Benign conditions (such as hemorrhoids) can also cause blood in the stool.Colonoscopy
Your doctor examines your rectum and entire colon using a long, lighted tube with a video camera at the tip (colonoscope). If polyps (benign growths that may lead to cancer) are found, they may be removed.Virtual colonoscopy
In this test, special X-ray equipment is used to produce pictures of the colon and rectum. A computer assembles these pictures into detailed images that can show polyps and other abnormalities.
Screening tests are recommended for individuals over 50 years old without any risk factors to detect pre-cancerous polyps at an early stage. Earlier screening is recommended for those with increased risk.4
Colorectal Cancer Prevention
There is no guaranteed way to prevent colorectal cancer from occurring. Nevertheless, these are some things you can do to lower your risk9,12:
- Go for regular screening - Colorectal cancer screening can find precancerous polyps and have them removed before they turn into cancer
- Have a balanced diet with more fruits, vegetables and whole grains, and less red meat and processed meats
- Stay active with regular exercise and maintain a healthy body weight
- Do not smoke
- Limit alcohol intake
Frequently Asked Questions (FAQ)
The likelihood of developing colorectal cancer increases as one grows older. The risk rises sharply from the age of 50, with around 90% of cases diagnosed in individuals aged 50 or over2.
The overall 5-year survival rate for colorectal cancer is 64%. However, the survival rate is significantly better for those with localised/ early stage disease, at 90%2. Regular colorectal screening allows early detection and higher chance of cure3.
Colorectal cancer is highly treatable and often curable, particularly when it is discovered in the early stages of the disease13.
The bowel is part of the digestive system. It is made up of the small bowel (small intestine), and the large bowel (colon and rectum). Bowel cancer most commonly occurs in the colon and or rectum, which is also known as colorectal cancer. In very rare cases, bowel cancer can also develop in the small intestine.

References
- National Registry of Diseases Office. Singapore Cancer Registry Annual Report 2020. Singapore, National Registry of Diseases Office; 2022.
- American Cancer Society. Colorectal Cancer Facts and Figures 2020-2022. Atlanta, American Cancer Society; 2020.
- American Cancer Society. Survival Rates for Colorectal Cancer. Accessed at cancer.org/cancer/types/colon-rectal-cancer/detection-diagnosis-staging/survival-rates.html on 4 July 2023.
- National University Hospital. Colorectal Cancer. Accessed at nuh.com.sg/Health-Information/Diseases-Conditions/Pages/Colorectal-Cancer.aspx on 4 July 2023.
- UpToDate. Colorectal Cancer: Epidemiology, Risk Factors and Protective Factors. Accessed at uptodate.com/contents/colorectal-cancer-epidemiology-risk-factors-and-protective-factors on 4 July 2023.
- Colon Cancer Coalition. Get the Facts about Colon Cancer. Accessed at coloncancercoalition.org/get-educated/what-you-need-to-know/colon-cancer-facts/ on 4 July 2023.
- Centers for Disease Control and Prevention. What are the Symptoms of Colorectal Cancer? Accessed at cdc.gov/cancer/colorectal/basic-info/symptoms.htm on 4 July 2023.
- American Cancer Society. Tests to Diagnose and Stage Colorectal Cancer. Accessed at cancer.org/cancer/types/colon-rectal-cancer/detection-diagnosis-staging/how-diagnosed.html on 4 July 2023.
- Gleneagles Hospital Singapore. Colorectal Cancer. Accessed at gleneagles.com.sg/conditions-diseases/colorectal-cancer/symptoms-causes on 4 July 2023.
- American Cancer Society. Treating Colorectal Cancer. Accessed at cancer.org/cancer/types/colon-rectal-cancer/treating.html on 4 July 2023.
- National Cancer Institute. Colorectal Cancer Screening (PDQ) – Patient Version. Accessed at cancer.gov/types/colorectal/patient/colorectal-screening-pdq on 4 July 2023.
- American Cancer Society. Can Colorectal Cancer Be Prevented. Accessed at cancer.org/cancer/types/colon-rectal-cancer/causes-risks-prevention/prevention.html on 4 July 2023.
- National Cancer Institute. Colorectal Cancer Treatment (PDQ) – Health Professional Version. Accessed at cancer.gov/types/colorectal/hp/colon-treatment-pdq on 4 July 2023.
- National Registry of Diseases Office. Singapore Cancer Registry 50th Anniversary Monograph – Appendices. Singapore, National Registry of Diseases Office; 2022.
