News & Articles

Open Dialogue with Breast Cancer Specialists

In Singapore, breast cancer is the number one cancer in women, with incidence rates rising rapidly. In the Open Dialogue with Breast Cancer Specialists public webinar, a panel of Breast Cancer Specialists comprising Dr See Hui Ti, Dr Wong Chiung Ing and Dr Georgette Chan share more about breast cancer and its management.
Like many cancers, breast cancer does not develop overnight. According to Dr See, before a cancer grows, we can modify our lifestyles to reduce risk factors causing the cancer and prevent the cancer from developing.
However, she emphasises that risk factors cannot be completely eliminated.
“The best way to manage risks is to screen and detect the cancer as early as possible so that it can be treated simply and effectively,” she explains.
Risk factors of breast cancer
Factors that increase risk for breast cancer:
- 5 children
- Age >40
- Low level of exercise
- Family history of breast cancer
- Not breastfeeding
- Stress
- High BMI
Factors that reduce risk for breast cancer:
- 1–3 children
- Hormone therapy
- Healthy diet
- Regular exercise
- Premature ovarian failure
- Vitamin D supplementation
- Low BMI
Understanding the modifiable factors that can increase and reduce risk for breast cancer can help women make positive changes to their lifestyle to prevent the disease.
Dr See highlighted that obesity in particular is a commonly overlooked cause of inflammation that can lead to breast cancer. In general, the greater the BMI, the greater the risk, while increased adipose tissue in the body can lead to a higher production of estrogen, which is linked to breast cancer.
To maintain a normal BMI, she recommended an optimal dietary strategy that combines higher protein intake, fibre for nutrients and carbohydrates for energy, with reduced sugar intake and moderate exercise.
However, she reminded viewers that despite best efforts to modify lifestyle factors, women can still get breast cancer. It is thus important to be aware of the signs and symptoms of breast cancer and how to screen for possible disease.
Screening for breast cancer
According to Dr Chan, a majority of lumps detected by breast self-examination (BSE) are benign. Despite this, she emphasised the importance of regular BSE to detect any changes in the breast.
Breast Self-Examination (BSE)
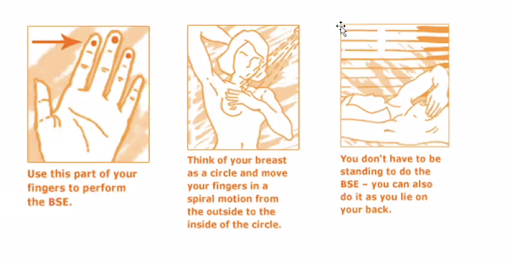
When to do? Once a month, one week after the start of your period
When to start? In your 20s
What to look out for? Lump(s), pain, asymmetry and skin changes on the breast, and any discharge, retraction, rash on the nipple
Should you feel something during BSE, Dr Chan recommends a triple assessment to assess the growth:
- Clinical examination
- Imaging (mammogram, ultrasound, MRI, tomosynthesis)
- Biopsy (core biopsy or fine needle aspiration, or mammographic or image-guided biopsy for non-palpable lesions)
In general, a mammogram is the best screening tool for breast cancer with improved ability to detect breast abnormalities before they are large enough to be felt during a breast exam. Statistics show that regular mammograms in women aged 40–69 showed a significant 41% reduction in risk of dying from breast cancer within 10 years, and a 25% reduction in risk of advanced breast cancer.
How often should you go for a mammogram? In Singapore, where the peak incidence for breast cancer is between 40–50 years old, those in this age group are recommended to screen once every year.
Those aged 50 and above are recommended to screen once every 2 years, while those with a family history of breast cancer should begin screening 5–10 years before the age of onset of cancer.
Advances in imaging have led to the development of 3D mammogram (also known as tomosynthesis). Here, several images are taken from different angles of the breasts to create a high resolution 3D picture that can detect more subtle changes to the breasts. This can be useful in women with higher breast density.
Dr Chan highlighted that regular screening should be affordable and informative. She advises women to see a breast specialist when they are symptomatic, have imaging abnormalities, or are at high risk of developing the disease.
Surgical treatment of breast cancer
Definitive breast cancer surgery focuses on the management of the breast and axilla, and breast reconstruction.
A mastectomy is a traditional surgical treatment for breast cancer, where the entire breast is removed. These days however, a wide excision or breast conservation surgery can be offered to certain cases (e.g. small tumours occupying one aspect of the breast) to preserve as much of normal breast as possible.
Dr Chan explained that while patients may require postoperative radiation therapy as a follow up, this method tends to be less scarring and cosmetically more appealing compared to traditional mastectomies.
However, not all patients may qualify for breast conservation surgery. These include patients with previous radiation to the breast, multiple areas of cancer, nipple involvement, poor cosmesis (large tumour, small breast), or have personal preference for mastectomy.
Typically, breast reconstruction is best done at the point of mastectomy so that all surgery is done in a single stage. The doctor will work with a plastic surgeon to reconstruct the breast using implants, the patient’s own tissue, or a combination depending on the patient’s preferences and the amount of work required.
Non-surgical treatment for breast cancer
Besides surgery, radiotherapy can be used to control and kill malignant cells as a form of localised treatment. For the systemic treatment of the primary tumour and metastatic disease, chemotherapy can be used to inhibit tumour cell growth and reproduction.
However, the limitation of chemotherapy is that it cannot differentiate cancer cells from normal cells, resulting in toxicity to other healthy organs, shares Dr Wong.
This is where novel treatments such as targeted therapy can offer more precise treatment. In hormonal therapy, oestrogen and progesterone receptors can be targeted to cut off the hormone supply that is stimulating the growth of the cancer. Compared to chemotherapy, this form of targeted therapy will target only malignant cells, since these cells express the oestrogen and progesterone receptors.
Other targets, such as HER2 targeted therapy for HER2-positive breast cancers and PARP inhibitors for breast cancers with BRCA mutations, can also be evaluated to offer more treatment possibilities to control the cancer.
Patients with triple-negative cancer (oestrogen, progesterone and HER-2 receptor negative) have limited targeted treatment options. However, there is still hope for them in the form of immunotherapy, which harnesses the body’s immune system to fight off foreign infections in a way similar to vaccinations against viral infections.
In summary, Dr Wong highlighted that the future of cancer treatment is personalised or tailor-made treatment that will enhance likelihood of response of treatment and reduce risks and toxicity. She reminded viewers that the earlier a patient is diagnosed and the earlier the stage of the cancer, the higher the chance of recovery for the patient. It is therefore crucial to go for regular mammograms and perform breast self-examination monthly for early detection of breast cancer.
| POSTED IN | Cancer Prevention, Cancer Treatments |
| TAGS | breast cancer, cancer awareness, cancer lump, cancer self-examination, mammogram, mastectomy, women (gynaecological) cancer |
| READ MORE ABOUT | Breast Cancer |
| PUBLISHED | 01 January 2022 |
