News & Articles

How CAR T-Cell Therapy is Changing the Landscape of Cancer Care

Chimeric Antigen Receptor (CAR) T-cell Therapy is making revolutionary breakthroughs in the field of Haematology by engineering immune cells to treat cancer.
For decades, the mainstay of cancer treatment has been surgery, chemotherapy and radiation therapy. While these treatment modalities continue to be the main pillars of cancer care, the emergence of targeted therapies, immune-based therapies, and cell therapies most notably CAR T-cell Therapy is shifting treatment paradigms in haematological malignancies.
CAR T-cell Therapy has been hailed as the next frontier of cancer treatment. Over recent years, it has shown promising results from numerous studies, including significant improvements in survival outcomes for the treatment of aggressive blood cancers such as B-cell Acute Lymphoblastic Leukaemia (B-cell ALL) and Diffuse Large B-cell Lymphoma (DLBCL).
But what exactly is CAR T-cell Therapy, and how is it changing the landscape of cancer care?
CAR T-cell Therapy: what is it?
CAR T-cell Therapy is a type of immunotherapy that harnesses the body's immune system to target cancer cells.
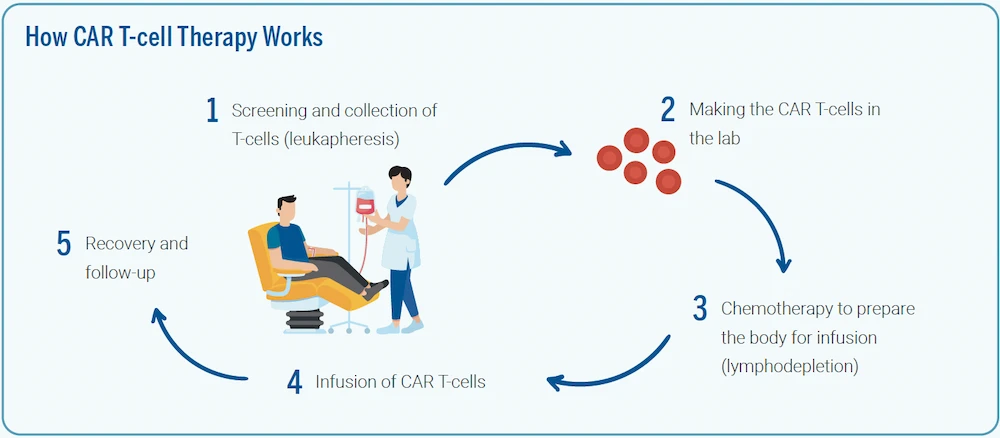
The entire treatment process takes about 3-4 months, depending on the patient's individual condition. It begins with a procedure called leukapheresis, where T-cells (a type of white blood cells) are drawn from the patient's blood.
The collected T-cells are transported under strict control to a CAR T-cell production facility where they are genetically engineered to produce CAR T-cells, which can identify and destroy the specific cancer cells like B-leukaemia and Blymphoma.
These CAR T-cells are then grown in a laboratory for several days before being transported back to the hospital to be reinfused into the patient. Once back inside the patient's body, the modified T-cells will be able to detect the cancer cells and destroy the cancer by harnessing the body's own immune response.
Following this procedure, the patient will be monitored closely in the hospital for any potential side effects and treatment response.
Is it safe?
Like any other treatment, CAR T-cell Therapy does not come without risks. In general, side effects of CAR T-cell Therapy include :
- High fever and chills
- Difficulty in breathing
- Nausea, vomiting and/or diarrhea
- Dizziness and lightheadedness
- Headaches
- Fast heartbeat
- Fatigue
- Muscle and/or joint pain
- Cytokine release syndrome (CRS) — an over-reactive systemic inflammatory response when CAR T-cells are eliminating cancerous cells.
- Immune effector cell-associated neurotoxicity syndrome (ICANS) — a syndrome that affects the central nervous system of the pat ient
Fortunately, these side effects are highly treatable and can be managed by a trained clinical care team.
How CAR T-cell Therapy is changing the treatment landscape
Recent studies on CAR T-cell Therapy have shown remarkable outcomes for the treatment of blood cancers.
In one study, the overall success rate in achieving remission with CAR T-cell Therapy is 60-80% for lymphomas and 70-80% for leukaemias1 . Many patients with previously relapsed blood tumours have also shown promising results with no evidence of cancer after receiving treatment.
What this means is that patients with blood cancer now have a potential life saving treatment option in the event that their disease is not responsive to standard treatment. This includes:
- Children and young adult patients from 2-25 years old with B-cell ALL that is resistant, and where a relapse has occurred subsequently or post-transplant.
- Adults with relapsed or refractory DLBCL who have not benefitted from at least two types of standard treatment.
- Adults with relapsed or refractory Follicular Lymphoma (FL) who have not benefitted from at least two types of standard treatment.
Looking ahead
As CAR T-cell Therapy is a relatively new area, there are some challenges to consider. This includes the selection of patients who can benefit from the treatment, logistical concerns, and the risk-benefit ratio of treatment for each individual patient.
However, it cannot be denied that CAR T-cell Therapy offers patients whose diseases have relapsed or previously failed to respond to standard treatment, a significant survival advantage that brings new hope for survival. CAR T-cell Therapy may be utilised for more B-cell lymphomas and may also be utilised earlier to give patients the best chance of survival.
In the years to come, we can expect more revolutionary breakthroughs in the area of cellular therapies as researchers continue to improve and refine the technology.
